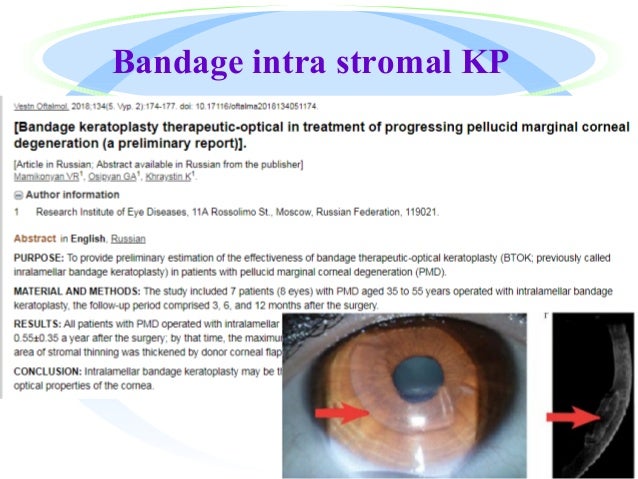
In this case report, we describe the presentation and surgical management of a patient with PMD. Some cases of graft rejection have been reported, and long-term use of topical and systemic steroids to mitigate graft rejection is required after lamellar keratoplasty. However, lamellar keratoplasty is a technically challenging procedure. Lamellar keratoplasty mitigates many of the complications of PKP. The disadvantages of PKP include graft rejection and long-term use of topical and systemic steroids. PKP involves the replacement of diseased cornea with a full-thickness donor cornea. Two common surgical treatments for corneal ectasia are lamellar keratoplasty and PKP. A variety of surgical techniques have been described for corneal ectasia, including intracorneal ring segments (ICRSs), full-thickness crescentic wedge resection in PMD, and lamellar keratoplasty, and penetrating keratoplasty (PKP). The topographic pattern often resembles a “lobster-claw.”Īs corneal ectasia progresses, the management changes from optical aids such as spectacles and contact lenses (CLs) to surgical intervention. PMD is a bilateral ectasia characterized by a peripheral band of thinning that incorporates the inferior quadrant of the cornea, with a central 1–2 mm zone of normal cornea. Keratoconus is the leading indication for corneal transplantation surgery worldwide. Combined treatments and improved screening could eliminate the need for surgical management in most cases of PMD.Keratoconus and pellucid marginal degeneration (PMD) are noninflammatory progressive ectatic corneal disorders, characterized by thinning of the corneal stroma that often leads to irregular astigmatism and a subsequent decrease in visual acuity. Corneal collagen cross-linking is especially exciting because it halts disease progression. Combining treatments such as ICRS, CXL, toric PIOL implantation, and refractive surgery is promising, but additional studies are needed to investigate their efficacy and safety.Īlthough little is understood about the etiology, pathophysiology, epidemiology, and genetics of PMD, new treatments are improving visual outcomes and reducing complications. CXL demonstrates effectiveness without complications, although data are limited and long-term results are needed. ICRS implantation can delay penetrating keratoplasty and improve contact lens tolerance, but does not treat the underlying process. Toric PIOL implantation is effective, but ectasia progression is a concern. Crescentic lamellar keratoplasty and TILK are effective, but technically difficult and without long-term results. CLWR is effective, but lacks long-term results.  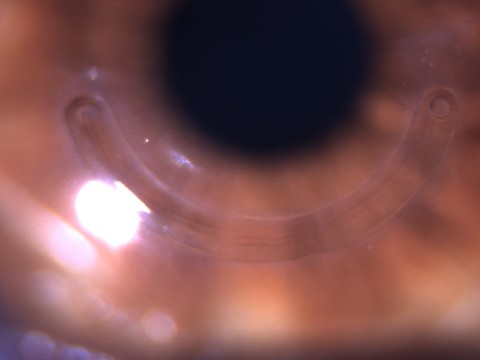
FTCWR has good visual outcomes, but with significant astigmatic drift. DALK provides visual outcomes similar to penetrating keratoplasty without the risk of immune-mediated graft rejection, but its complexity and relative novelty limit its acceptance. Penetrating keratoplasty is the treatment of last resort in PMD and is effective, but with considerable complications. Reported data for each treatment is presented. This is the first review article looking at the literature specific to PMD. To review and evaluate current and future directions in the diagnosis and surgical management of pellucid marginal degeneration (PMD), including penetrating keratoplasty, full-thickness crescentic wedge resection (FTCWR), deep anterior lamellar keratoplasty (DALK), crescentic lamellar wedge resection (CLWR), crescentic lamellar keratoplasty, tuck-in lamellar keratoplasty (TILK), toric phakic intraocular lens (PIOL) implantation, intrastromal corneal ring segment implantation (ICRS), corneal collagen cross-linking (CXL), and combined therapies.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
